7 Misconceptions about incontinence
Urinary Incontinence is often misunderstood and because it can be embarrassing it is not talked about. This causes millions of people to mistreat and mismanage their symptoms. So, I have put together a list of common misconceptions people have about urinary incontinence, in hopes that it encourages people to talk about their symptoms, properly take care of them, and raise awareness.
Misconception #1: Only older people get it
Urinary incontinence can affect people of all ages. However, the risk does go up as a person ages, but it is not an inevitable part of aging. In fact, one study in Reviews in Urology, found the prevalence of incontinence in women being young adults 20-30%, middle age 30-40%, and elderly 30-50%. As the body ages, it changes and this can lead to an increased risk of incontinence. Menopause and childbirth have been shown to increase the risk of urinary incontinence. In males, prostate problems, such as enlarged prostate and prostate cancer, have been linked to an increased risk of urinary incontinence.
Misconception #2: There is nothing to be done for urinary incontinence
There is a range of management and treatment options available to you or a person you are caring for. They include:
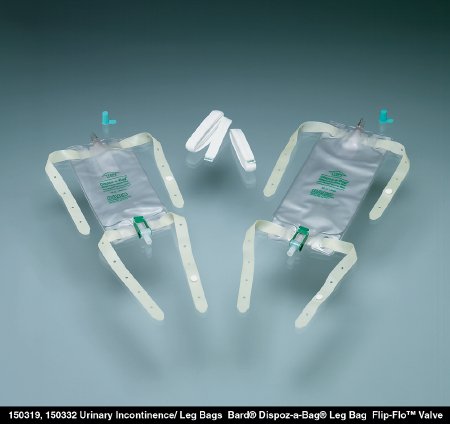
- Absorbent products and other devices: An external catheter, or condom catheter, is a device that goes over the penis to control leakage. A Pessary is a device that is inserted into the vagina to prevent unwanted leakage. Protective pads and panty liners, along with briefs and diapers can help manage incontinence. There are also creams and wipes to maintain healthy skin and comfort. Bed pads are available and usually used at night. Our staff can help with any questions you may have about products. Consult your doctor for a primary assessment.
- Behavioral treatment: depending on the type of incontinence a range of lifestyle changes can help, such as changing the food you eat or alcohol consumption. An exercise called Kegels, which strengthens pelvic floor muscles, can help. Check out Cleveland Clinic’s “Kegel Exercises” for more information. Bladder training/retaining is the process of gradually increasing the time intervals between urinating. This means that you schedule your bathroom breaks, and progressively schedule them farther apart. It is also recommended to void your bladder before leaving your home, even if you feel like you don’t need to. This will decrease your chance of unwanted leakage. Living a healthier life with proper exercise and diet can also reduce the risk of developing urinary incontinence. Check out WebMD’s home treatments, here.
- Medications: There are multiple medications that are used to treat incontinence which vary depending on the type. Consult a doctor for proper medication. If medications do not work, Botox can also be injected into the bladder muscle to improve spasticity.
- Surgery: This is often the last resort. Ask your doctor what your options are and what they recommend.
One study shows that when compared to doing one of the above, doing combination therapy significantly reduces incontinence episodes, improves quality of life, and results in greater treatment satisfaction directly after treatment.
As people become more familiar and comfortable with their urinary incontinence, more options will emerge. Progress doesn’t happen with people staying silent. Within the last few years, incontinence has gotten much more recognition, leading to innovations and progress in management and treatment.
Misconception #3: It isn’t a common problem
Urinary Incontinence happens to more people than you may think. In recent years, however, the stigma surrounding incontinence has begun to lift, but we still have a long way to go. Don’t be afraid or embarrassed to talk to your doctor or nurse, they are there to help and you aren’t the only one. It has been estimated that more than half of adults will experience incontinence at some point in their lives.
Misconception #4: Drinking less fluid improves urinary incontinence
Many people think that limiting the amount of fluid intake will improve symptoms. Although drinking too much can lead to leakage, drinking too little can have the same effect. Tomas Griebling, MD, MPH, vice chair of the department of urology at the University of Kansas Medical Center in Kansas City, says, “When you don’t drink enough water, the urine becomes more concentrated and that can be irritating to the bladder and increase urgency.” You can, however, manage your fluid intake by choosing when to consume liquids and avoiding liquids that can make symptoms worse, like caffeine and alcohol.
Misconception #5: Incontinence does not occur in men
Urinary Incontinence is more common in women, but it also occurs in men. It is estimated that 3-11% of males experience urinary incontinence. The exact number of males living with urinary incontinence is unknown.
Misconception #6: Kegels are only for women
Kegels are an exercise that is used to strengthen the pelvic floor muscles. This is done by contracting the muscles in the pelvic region 30 to 100 times a day. It has been said that in men, Kegels should resemble the feeling of the contraction required to hold back gas. It has been shown to improve symptoms, so whether you’re a male or female get to ‘kegeling’!
Misconception #7: Surgery is the only way to treat urinary incontinence
Surgery can treat urinary incontinence, but it is often the last resort. Behavioral changes have been shown to treat urinary incontinence. This includes, but is not limited to, living a healthy life, quitting smoking, bladder control exercises, and avoiding triggers. Medications have also been found to treat symptoms. These medications differ depending on the type of incontinence, so talk to your doctor.
There are many options out there and the first step is to talk to your healthcare provider. Just remember you are not alone.